
High-Denial CPT Codes That Hurt Reimbursement Most: Why Healthcare Practices Keep Losing Revenue
In today’s healthcare reimbursement environment, claim denials are one of the biggest threats to consistent cash flow for physician groups, specialty clinics, urgent care centers, and hospital-based providers. Even practices with experienced billing teams often struggle because certain CPT codes face repeated scrutiny from commercial insurers, Centers for Medicare & Medicaid Services edits, and payer-specific policy changes.

How Small Medical Practices Can Reduce Revenue Leakage Through Better Medical Billing
Small medical practices across the United States face growing financial pressure from rising operating costs, payer complexity, staffing shortages, and delayed reimbursements. While many providers focus heavily on patient care, one of the most overlooked threats to profitability is revenue leakage—small but repeated losses in reimbursement caused by billing inefficiencies, coding errors, missed charges, and poor follow-up.

Why Nephrology Practices Are Outsourcing Medical Billing to Improve Revenue Cycle Performance
Nephrology practices across the United States are facing growing financial pressure as reimbursement rules become more complex, payer requirements continue to change, and claim denials increase for kidney-related services. From chronic kidney disease management to dialysis billing and hospital rounding, nephrology involves highly specialized coding that directly affects revenue.

10 Medical Billing Best Practices Every Healthcare Provider Should Follow to Improve Cash Flow
In today’s healthcare environment, strong cash flow is essential for every provider—from small private clinics to large specialty groups. Even when patient volume is strong, delayed reimbursements, claim denials, coding errors, and poor billing workflows can create major financial pressure.

Telehealth Billing Rules for Behavioral Health in 2026: What Providers Must Know
Telehealth has become a permanent part of behavioral healthcare delivery in the United States. Mental health providers increasingly rely on virtual visits to treat patients with conditions such as anxiety, depression, substance use disorders, and PTSD. However, while telebehavioral health remains widely reimbursed in 2026, billing rules have evolved, and providers must follow updated payer guidelines to avoid claim denials and reimbursement delays.

How Large Medical Groups Can Reduce Revenue Leakage Through Centralized Medical Billing
Large medical groups operate in one of the most financially complex environments in healthcare today. With multiple providers, specialties, service locations, and payer contracts, even a small breakdown in billing processes can create major revenue leakage over time. For physician groups handling thousands of claims each month, lost revenue often happens quietly—through missed charges, coding inconsistencies, delayed submissions, underpayments, and unresolved denials.

Hidden Revenue Risks: How Misusing Non-Billable CPT Codes Causes Claim Denials
In today’s healthcare reimbursement environment, even small coding mistakes can create significant financial consequences for medical practices. One of the most overlooked causes of denied claims is the misuse of non-billable CPT codes. Many providers assume that if a procedure or service is documented, it can automatically be billed to an insurance payer. In reality, certain CPT codes exist for reporting, internal tracking, bundled services, or documentation support—but are not separately reimbursable.
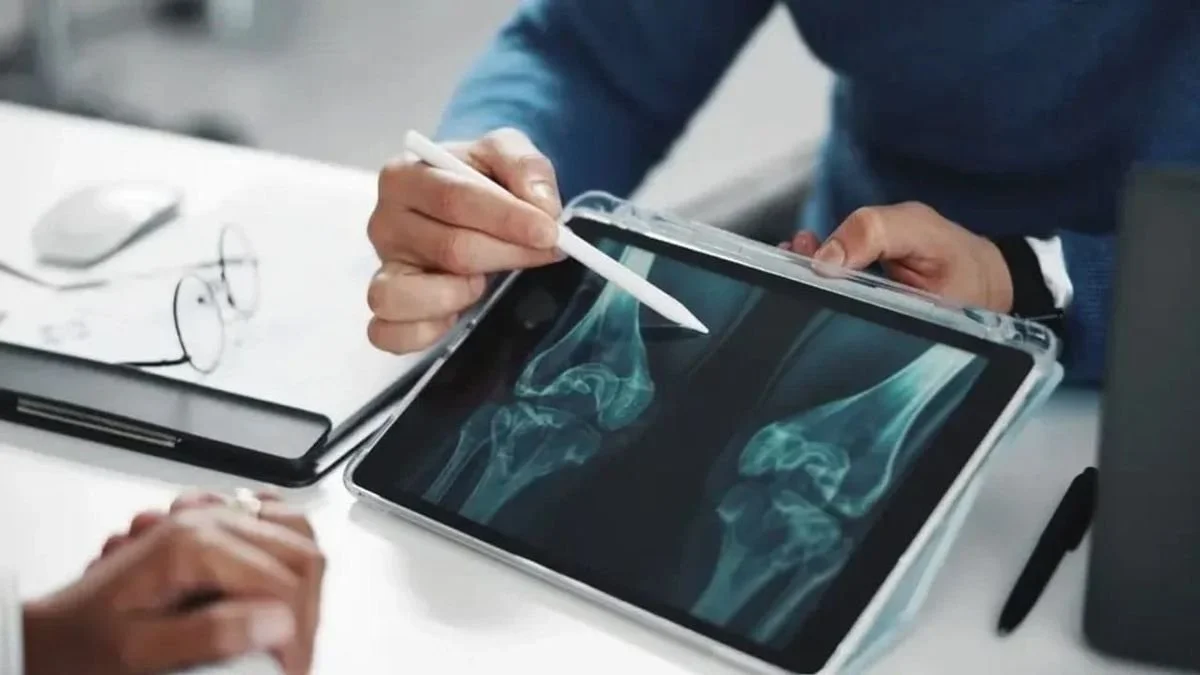
Bundled Payments for Joint Replacement: Billing Challenges Orthopedic Practices Must Solve
Orthopedic practices across the United States are facing a major reimbursement shift as bundled payment models continue to expand in joint replacement care. Programs led by Centers for Medicare & Medicaid Services have changed how providers are paid for procedures such as total knee and hip replacements, placing greater financial accountability on hospitals, surgeons, and billing teams. Under bundled payments, providers receive one fixed reimbursement for the entire episode of care instead of separate payments for every service delivered.

CPT 92933 vs CPT 92928: Coding Differences That Impact Reimbursement
Accurate cardiovascular procedure coding is one of the most important parts of protecting reimbursement in interventional cardiology. Even small coding mistakes between coronary intervention CPT codes can trigger denials, underpayments, payer audits, and delayed revenue.

How Accurate CPT Coding Increases Revenue for Healthcare Practices in 2026
In today’s healthcare environment, revenue pressure is increasing while payer scrutiny is becoming more aggressive. In 2026, healthcare practices across the United States are facing tighter reimbursement policies, stricter documentation requirements, and more frequent claim audits. Under these conditions, accurate CPT coding has become one of the most important drivers of financial performance for medical practices.

How Medical Billing Data Can Predict Cash Flow for Healthcare Practices in 2026
Healthcare practices today operate in an increasingly complex financial environment. Between evolving insurance regulations, payer delays, coding updates, and rising operational costs, maintaining stable cash flow has become one of the biggest challenges for medical providers.
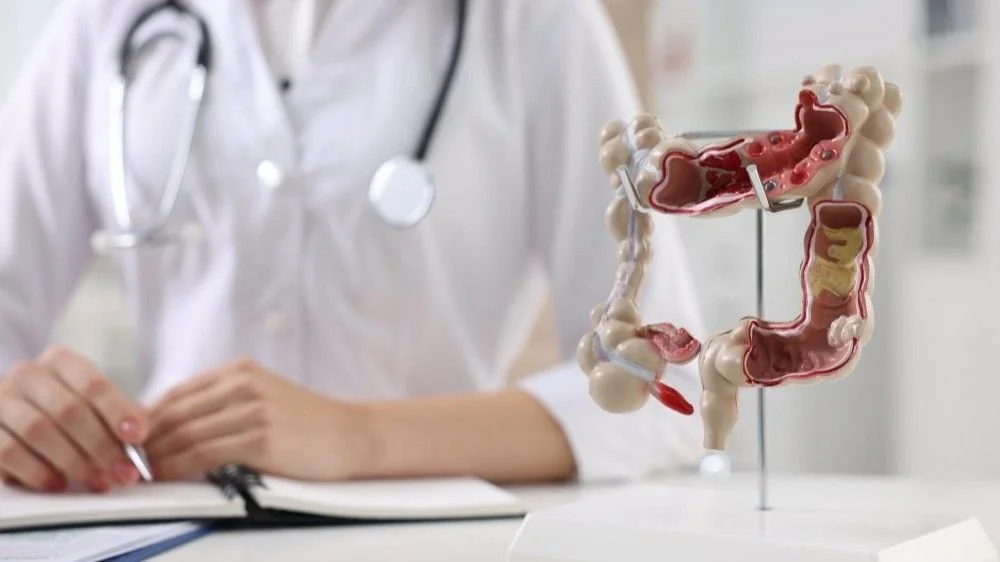
Why Gastroenterology Practices Are Outsourcing Medical Billing in 2026
The healthcare industry is becoming increasingly complex, and gastroenterology practices are facing growing administrative and financial challenges. From complicated procedure coding to rising claim denial rates, managing billing internally has become a difficult task for many practices.

Value-Based Care & Its Impact on Medical Coding and RCM
The U.S. healthcare industry is steadily shifting from the traditional fee-for-service model to value-based care (VBC). Instead of paying providers for the number of services delivered, value-based care focuses on patient outcomes, quality of care, and cost efficiency.

How Incorrect CMS M-Code Reporting Is Quietly Reducing Healthcare Practice Revenue in 2026
Healthcare reimbursement is evolving rapidly as the industry shifts toward value-based care and quality-driven payments. In 2026, quality reporting through CMS programs has become a critical factor that directly impacts how much healthcare providers are paid.

Top Revenue Cycle Management Strategies for Healthcare Practices in Utah
Healthcare providers across Utah face increasing challenges when it comes to managing revenue cycles efficiently. From rising claim denials and complex insurance regulations to staffing shortages and delayed reimbursements, medical practices must adopt smarter strategies to maintain financial stability.

Why Federally Qualified Health Centers (FQHCs) Are Outsourcing Medical Billing in 2026
Federally Qualified Health Centers (FQHCs) play a vital role in delivering affordable healthcare services to underserved communities across the United States. These community-based clinics provide comprehensive medical services regardless of a patient’s ability to pay. However, behind the mission of improving public health lies a complex operational challenge: medical billing and revenue cycle management (RCM).

Specialty-Specific Medical Billing Services: Which Practices Need Expert Billing the Most?
In today’s rapidly changing U.S. healthcare landscape, medical billing is no longer a one-size-fits-all service. Every specialty has unique coding rules, payer policies, compliance requirements, and reimbursement challenges.

Top Revenue Cycle Management Strategies for Healthcare Practices in Montana
Revenue Cycle Management (RCM) is the financial backbone of every healthcare practice. From patient registration to final payment collection, every step directly impacts cash flow, compliance, and profitability.
For healthcare providers in Montana, RCM comes with unique challenges—rural operations, limited staffing, payer complexity, and frequent reimbursement delays. Many practices face high denial rates, administrative burden, and cash flow instability due to inefficient billing processes.

Insurance Credentialing for Mental Health Providers: Avoid Delays and Get Paid Faster
In today’s competitive behavioral health landscape, insurance credentialing is the gateway to consistent revenue. Whether you're a psychiatrist, psychologist, therapist, or mental health clinic, delays in credentialing can mean months of lost income, denied claims, and frustrated patients.

Is Your Kansas Practice Losing Revenue? 7 Signs You Need Professional Medical Billing Services
Running a successful medical practice in Kansas requires more than delivering quality patient care. Behind every appointment, there’s a complex billing process that directly impacts your revenue. Unfortunately, many practices unknowingly lose thousands of dollars every month due to inefficient billing systems, coding errors, and delayed reimbursements.
